 Chapter One: Discharge: When we were discharged from the hospital, I truly believed hospital life was over; we were now HOME so naturally I thought my life would now be a typical mat leave. When we got home, Theo was struggling to drink his fortified breast milk and when he consumed an adequate volume of milk, he would vomit more than he consumed. My days were consumed with trying to feed him to get the volumes of milk that he needed and administering medications every two hours. Needless to say, there was ZERO sleeping happening. Any time Theo would sleep for 2-3 hours, the slightest stir would make me jump to A) make sure he was a alive and B) just maybe this time, he was hungry and would drink his milk. We were constantly between our family doctor’s office, our pediatrician and Sick Kids regarding Theo’s weight gain. I literally talked to his dietician and nurse practitioner weekly, and I always needed to provide the daily/weekly volumes of milk he was consuming. It was so stressful and exhausting; my world revolved around counting milliliters. I hated feeding him, and I couldn’t bare the thought of leaving the house to experience some of the activities I had anticipated doing as a new mom as the times did not jive with his feeding schedule. Not to mention, I was only getting about maybe 2 hours of sleep a day….I was a mess. I was completely emotionally, physically and mentally exhausted. And when I did try to meet up with even the closest of friends, all the moms talked about was what their baby ate, how fast they were growing and how they were sleeping. I felt like no one understood my struggles. Usually when I explained my hardship to friends, even the new mom friends I had made, they would try to talk about other things, but when you have a baby, all you talk about is baby stuff….which usually includes sleeping, eating, and growing. But when my baby was greatly struggling in all these areas, I felt like a complete failure. I began to isolate myself more and more and I hated leaving the house. SIDENOTE: truth is, having a baby completely changes you but having a sick baby is something no one can prepare for and few people understand. The difference in people’s reactions and consideration of mine and my baby’s circumstance was not something I had anticipated. People who I thought would be there for me disappeared while others showed up with unimaginable support. I lost friends who I thought were like family, and unfortunately, I had to cut people out completely for my own well-being. I am a people pleaser by nature and hate confrontation so this change in my social network was an additional unneeded stress. I found an amazing therapist to help me through but what I wish I knew earlier was that I didn’t need to pretend I was okay when I wasn’t. I didn’t need to make an effort to stay connected to people who could not understand what I was going through. At the end of the day, not everyone in your life will provide you with the support that you need but there’s no shame in leaning heavily on the people that can.  Chapter Two: NG Tube (feeding tube that goes into the nose bringing milk directly to the stomach) Feeding was very distressing for both me and Theo and he was not eating enough to gain weight at home. We were admitted back to Sick Kids for a week where we met with our team and the surgeon recommended an NG Tube as he was termed under the category of Failure to Thrive. Who the FFFF comes up with these names!? To me Failure to Thrive meant failure as a mom. Simply put, NG tubes suck! The NG tube went in and we were taught how to manage it at home. Basically we would feed Theo his milk from a bottle orally and then add the remaining milk that he did not drink through the tube. Having an NG tube with a very active toddler was challenging to say the least. My husband and I would always be amazed at his abundance of energy despite his low calorie intake and lack of sleep! At one point we were even told not to let him go in his Jolly Jumper because he was burning too many calories! Jokes aside, the NG Tube is a scary thing to live with. I knew it was only a matter of time before he pulled it out and I was terrified of him sleeping with it and getting it wrapped around his neck; this worry only exacerbated my difficulty sleeping at night. When we got home from the hospital the first thing I did was put a post on my Facebook page to see if any of the nurses I knew or friends or family had nurses that live near me that could help me put the NG tube back in if/when it came out. The hospital taught us how to put it back in but I knew I couldn’t do it on him myself. So of course one week after being home with the NG tube, it came out. We had gone to a nurse’s house and she was absolutely amazing at comforting (me) and Theo and put the NG tube back in. But I was distraught. Theo hated the tube and was always trying to pull it out. My worries and anxiety continued to increase; why couldn’t my baby eat? People kept sending me ideas; “have you tried this? have you tried that…”, the suggestions became irritating - yes of course I’ve tried everything but nothing is working! The NG tube was short-lived as we were not comfortable with it and it was causing distress for all of us.  Chapter Three: G-Tube: As mentioned above, despite our best efforts, the NG Tube was not working for our family. At Theo’s first birthday, the poor little guy only weighed 14 pounds. I had no idea at the time how incredibly small this was for a one-year-old. I had very little to compare to and he was still my perfect little baby. At this point, the G-tube was presented to us as the miracle solution to all our problems. It was explained to us that it may be our ultimate cure for helping Theo gain weight. Literally the day after his first birthday, he went in for G-tube surgery. Theo had been through so much and I was so worried that he was going to die during the procedure; it was absolutely terrifying but the procedure was actually pretty quick. We were extremely concerned about having a baby with a feeding tube but we felt confident that this was going to help him. Theo still at this point, did not sleep- like at all. I mean it was a good night if he did a three hour stretch at 14 months. We were assured that the G- tube should help fill up his belly, decrease reflux and indigestion, improve intake of his medication as it would go directly into his stomach and thus hopefully help with sleep. Well.... let’s just say the plan failed!  -SIDENOTE: I want to point out that Theo’s condition was extremely complicated. The more I talk about his story, I am in awe of how he survived the first year of his life. When we would go back to follow up clinics, our surgeon would see him and literally just smile at me and say “Jessica he’s a miracle”. In saying that, the details that I am providing is solely based on MY experience with feeding. Theo’ experience is not normal or typical but I’m writing about it so people have a better idea of what feeding will be like with a G-tube. Also, I think it is important to point out the ugly truth because I was completely oblivious to many of the challenges that arose and I think it’s important to be prepared so that if things do not go smoothly, you have tools to get through it. And you will get through it <3 Chapter Four: A G-Tube at Home: Once we were home, a nurse came to the house to look at the bandage and change the gauze surrounding the G-tube. Unfortunately, we had another rare and inexcusable situation where the nurse cut a stitch that was not supposed to be cut yet as it was still holding the G-tube in place. Luckily, there was no damage done to Theo or his feeding tube but it was an ugly situation. I had the crisis intervention team over from the community support service known as the LHIN and I was livid beyond words (not to mention STILL NOT SLEEPING). We had gone through so much and had placed so much trust in the nurse looking after our baby and she totally messed up. Again, I felt like this was something that was my fault and I didn’t know how to advocate. In saying that, when the nurses come to your house, obviously you do not want to be argumentative, but you need to be strong and assertive. I wish I would’ve asked: how many times have you done this on a baby? Can you tell me what you’re doing step-by-step and why you’re doing it? What should I expect after you go? Who can I contact if X,Y or Z happens? After this crisis was dealt with, we had a phenomenal nurse come to treat Theo and she ended up being our weekly nurse. You have a weekly nurse to assist with wound care as there is literally a hole on the outside of your child’s body that directly goes into their stomach. This wound, despite the best of efforts, can get infected and needs to be regularly seen by a health professional. She was phenomenal. She walked us through every step and told us everything she was doing and why she was doing it. She also reassured us that we were doing a good job in terms of taking care of his wound and this reassurance meant the world to me. When his wound would get gunky, as it often did, and sometimes infected, she would remind us that these things happen, it’s not our fault and these are things to do to help make it better. This nurse had a profound impact on easing my anxiety and providing thorough care for our family. Below are videos that support G-Tube wound care: https://akhpub.aboutkidshealth.ca/Article?contentid=3019&language=English&hub=tubefeeding https://www.aboutkidshealth.ca/article?contentid=2907&language=english  Chapter Five: Supplies: Getting a G-tube means needing a ton of supplies. There wasn’t much coverage for getting the necessary supplies and it was quite costly. We didn’t reach out for help but looking back on it, we probably should have. Financially, we were doing OK but when family and friends help out with financial medical costs it’s just one less burden to think about. The hospital will provide you with a list of items you need, the main ones being the pump, bags, gauze, tape and syringes. We were like dear in the highlights and bought everything. Don’t over do it, if you need more supplies, you can go back and get them ;) Chapter Six: Tips for Living with a G-Tube: -Ask for help! We trained our parents on how to use the tube. I originally thought they would be uncomfortable doing it but they were eager to learn and help. Remember the people that love you, want to help you, so let them. You can’t do this all alone, and it’s good to train your family on how to use the tube so they can support you. You’ll have training by the hospital and your family can also attend the training (pre-Covid). - Once your child gets a G tube, you’ll be assigned a specific G-tube nurse from the hospital. BECOME BFFs with your G-tube nurse immediately – they will become your lifeline! They are super knowledgeable on the tube and can walk you through simple corrections that make huge improvements over the phone at home if something is off. - How to use a G-tube: just like the NG Tube, Theo would eat what he could orally via a bottle and then we would top up the milk through the tube. The G-Tube allowed us to also feed him greater volumes of milk. We found that when Theo napped and was in an elevated position, he was less likely to have reflux. I would often go for a long walk with him in the morning and the afternoon (even in the winter) by connecting the G-tube bag with a safety pin to the side of our stroller. Also, if I was in transit, I would hook up the G-tube and again just use a safety pin to attach the bag to his car seat. (I would only feed him in the car if it was a short distance and I would never go on the highway in case he would vomit). Another option is to have them sitting in a high chair and have some finger foods they can play with. At approximately 16 months, Theo didn’t eat any solid food and drank very little milk. Like, I mean he didn’t even swallow a cheerio! We would have food in front of him and he would just play with it. For example, we would place food items such as vegetable sticks, French fries, pretzels...etc with dips for him to just play with and then slowly start to bring to his mouth. It was explained to us by our phenomenal Occupational Therapist that this was a huge step. Did you know there’s actually 20 steps to eating?! So having your baby just explore food is a huge step. As well, getting them to explore food while their G-tube is filling up their belly helps their brain to connect eating / hunger to the feeling of being full. -Find an Occupational Therapist (OT) you work well with. At the beginning we had several different OT‘s checking in on Theo. I don’t know when or how it happened but one day an OT was sent to our house and it was like an angel came down from the heavens. I truly don’t think I could’ve gotten through my experience without her support. She played a vital role in Theo’s motor development and progression with eating. She taught me how to advocate for him and provided a variety of options and tools to get him to eventually learn to eat independently. -Find a G-tube support group. When I first joined the G-tube support group on Facebook I felt such relief because people were posting their frustrations, victories and helpful ideas regarding using the tube and wound care. I no longer felt alone; I remember one particular post where a mom made a onesie with a G-tube cut out in it that said: Yes, I’ve tried that! And I thought YESSSS...these are my people...they get it! -Something to hang your G-Tube bag on: one item that was essential for feeding Theo with a G-tube was a paper towel rack holder. When he was sitting in a high chair or sitting and playing with blocks for the floor, I used a paper towel holder to keep the bag elevated (the bag needs to be elevated to flow). Having a small paper towel holder was a great way to keep the bag elevated and was portable. -Travelling with a G tube: The first time you leave your house will be extremely daunting even if it’s just for a walk or just to your parents house. MAKE A LIST! Write down everything you need to hook up a feed and have extra supplies of everything (except for the pump). With Theo, we did end up driving to a cottage that was four hours up north. The hospital was about 50 minutes from the cottage but I felt comfortable going as one of my closest friends was there and she is a nurse. A G-Tube can easily come out; if it does come out, the G-tube has to go back in the stoma (hole in the tummy) in a certain amount of time before the skin closes. When you’re trained on how to use the G-tube, they teach you how to insert it back into your child. Don't get me wrong, I love watching surgery shows but I am not a doctor or a nurse nor could I do something like that to my own kid. I got my friend to repeatedly watch the video on what to do if it came out and she felt comfortable that (God forbid it came out) while at the cottage she could secure it until we got to the hospital. We also travelled to the US with his G-Tube as I was in a very close friend's wedding. My husband, parents and friend who is a nurse were with us and having people who know and understand the tube was important in a new setting. Chapter Seven: What To Do When the G-tube Comes Out: Before knowing what our journey would be like with Theo, my world traveler Grandmother generously booked me, my sister, my mom and my aunt a trip to Paris for one week! Prior to having Theo, we knew he would be approximately 16 months at the time of the trip and it seemed totally manageable to be halfway around the world for one week. However, at the time of the trip, I felt like I couldn’t leave but my husband, dad and mother-in-law all assured me that they would all team up and hold down the fort while I was gone for the week. After all, I desperately needed the rest. One night while I was FaceTiming with Theo, my hubby and dad, they were being really awkward on the phone. I thought it was just because they were exhausted from the around-the-clock-care Theo needed but when I got home, my hubby told Theo to show me the teddy bear he had gotten while I was away. I knew in seeing the teddy bear that Theo had been in an ambulance because he got the same one a couple of times prior. My hubby explained what happened as my mouth dropped open… Holy shit… His tube… Came out… While I was in fucking Paris!? I was consumed with guilt and completely shattered that I wasn’t there during this crisis but at the end of the day, it happened, it sucked and it was put back in and he was fine. Sorry to say this but the G-Tube will probably come out. Prepare yourself; have a plan! We didn’t go ANYWHERE without Theo’s emergency kit and letter. The emergency kit is a temporary tube that replaces the proper G-Tube to keep the hole in the skin open. The letter contained specific instructions on how to place it in a toddler based on Theo’s specific anatomy. When Theo started preschool with his G-tube, we decided that if the tube came out at school, the school would call an ambulance and us immediately and then provide EMS with the emergency kit and letter. Once Theo was stable, either the ambulance or us would take him to Sick Kids (lucky we are only an hour away) to get a new tube properly placed. Being prepared for different scenarios brought us a lot of reassurance and reduced the guesswork in emergency situations. Of course, there is no plan for some situations but remember to stay calm, breathe and like everything else that you’ve gone through, you and your baby will get through this too. SIDENOTE: I want to point out that Theo’s condition was extremely complicated. The more I talk about his story, I am in awe of how he survived the first year of his life. When we would go back to follow up clinics, our surgeon would see him and literally just smile at me and say “Jessica he’s a miracle”. In saying that, the details that I am providing is solely based on MY experience with feeding. Theo’ experience is not normal or typical but I’m writing about it so people have a better idea of what feeding will be like with a G-tube. Also, I think it is important to point out the ugly truth because I was completely oblivious to many of the challenges that arose and I think it’s important to be prepared so that if things do not go smoothly, you have tools to get through it. And you will get through it <3
0 Comments
 Chapter One: Pumping My son Theo was born with gastroschisis, a birth defect in which the intestines grow outside the baby’s body. As soon as my son was born, even before I was able to see him, the nurses started talking to me about pumping. I was literally told “Jessica, your only job is to pump right now”. Theo’s condition was very complex and I felt completely helpless as his mother. I felt that the only thing I could really do for my baby was to pump and I soon found that pumping consumed my life and became a source of my anxiety. In saying that, I don’t regret pumping by any means BUT….at the same time I look back and wonder why was that enormous pressure placed on me? Every mom has to make the decision that’s right for her and her baby and while I choose to pump, you need to do what’s right for you. My experience with feeding Theo was traumatic and while I’m not trying to scare other mom’s who may be experiencing similar struggles, I want to provide recommendations and suggestions for pumping/breastfeeding that I wish I someone shared with me. I’m not a medical professional so all recommendations are just based on my personal experience. STEP 1: GET A PUMP AND A PUMPING BRA!!! Prior to pregnancy, buy a high quality pump. Many insurance plans cover them with a doctor's note when you have a high risk pregnancy. If purchasing one is not an option, they can be rented for a reasonable price from the hospital where they are sterilized daily. Learn how to use the pump BEFORE the baby comes out. DADDY/your partner: LEARN how to clean and sterilize the kit (as that will be a huge help for mama). I definitely didn’t do that the first time; I was trying to pump while learning how to put the damn thing together and I had no clue what the hell I was doing. After an untraditional birth the last thing you want to be dealing with is how to use the pump correctly. Prior to your induction/due date, explore the pump! Attach the pump with the correct cords and play with the settings. Then put it on your boobs - TEST IT OUT! Learn how to attach the pumping bra to the pump. I didn’t use a pumping bra until I got home from the hospital with Theo and it was a total game changer as you are hands free! The first setting will probably be uncomfortable for a while. However, once your milk starts coming in, you will be able to increase the suction comfortably. STEP 2: Buy a sterilization kit. I bought one that went in the microwave and really liked it because it was compact and easy to use. There are also disposable bags you can use that are convenient when on the go. Have all of this ready to go in advance. 3. WHEN TO START: Once you are settled after the birth and feel somewhat composed, try to put the pump on your breasts. With Theo I produced NOTHING for about three days. I was panicking and felt like a failure. At the same time, NO one was encouraging my efforts and reminding me that my situation was nowhere close to a normal experience. OF COURSE my milk wasn’t coming in; my baby was in critical care, literally fighting for his life and I was stressed beyond belief. It is important to remember women’s milk supply usually comes in because moms typically hold the baby after birth. With the stress of having your baby covered in tubes and wires, followed by a perhaps undesirable birth, it is only natural that your body responds by saying, WHAT THE FFF?! WHERE’S THE BABY??? I’M CONFUSED! You’ll most likely be told to put the pump on your breast every two hours. As a natural rule follower, I became obsessed with my exclusive pumping role and being on-time to the very minute to pump. Well guess what….after giving birth you might not be able to walk, you might not even be staying in your house and pumping rooms are not always available at the hospital when you want to pump. So all you can do is try your best to pump on the two hour mark. If you're 20 minutes or an hour behind, take a breath, you’re living through unimaginable time with your baby and it’s fine to move at your own pace. The nurses and lactation consultants will be asking you about pumping. Some are kinder than others. Remember this is YOUR experience, NOT theirs. Listen to your body and just keep trying your best. SIDENOTE: I’m not sure why our society doesn’t talk about this but breast-feeding/pumping is hard! It’s so hard that there are specialized trained nurses whose main role is to teach women how to breast-feed. Don’t get me wrong, there are multiple important and amazing parts of breast-feeding but I think we should highlight that if it was so damn easy and natural, why is it someone’s career to just teach women how to do it? 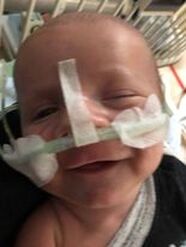 4. WHERE TO PUMP IN THE HOSPITAL: The NICU at Sick Kids is unimaginably small...hence the NEED for a new SickKids building. It’s recommended to pump by the bedside to improve milk production as you are in close proximity to your baby. Nurses can provide covers for privacy, don’t be afraid to ask. At first I was completely uncomfortable pumping by the bedside with Theo. I felt that the curtains didn’t give me enough privacy and I didn’t know what the hell I was doing. When my second born, Christian, was also born with gastroschisis and I found myself in the same situation, I often asked to pump by the bedside. I preferred it much more the second time around as I didn’t need to wait for a room, I could consistently pump on the approximate two hour mark during the day and I felt a little more connected to Christian when pumping. Also, the great thing about pumping beside the bedside is that you can provide mouth care to your baby immediately. Mouth care is provided when your baby is not receiving feedings by breast or bottle. You swab the inside of your baby’s mouth with small amounts of your colostrum then later breast milk. I really enjoyed doing this hands-on care for my boys and it helped me to feel connected to the boys and feeling like a mom. So many aspects of becoming a mom were taken away from me and this small experience helped me to feel like I was a mother and I could do something for my baby. Also my husband could participate in mouth care which provided a bonding experience for him as well. Both my boys did not receive milk from a bottle or breast until they were approximately two and a half months old. With regards to Theo, he went through a lot at the beginning; in the first four hours of his life, he needed an immediate surgery and my husband was told he may not make it. Doctors kept telling my husband and I that our son’s case was extremely complicated but after the first week, he started improving despite his unhealthy bowels outside his body. After the two week mark, we got a call in the middle of the night to come to the hospital right away. Theo needed a large blood transfusion and we were told he may not make it through the night. Later we were told he was septic, had E.Coli in his blood as well as a condition called NEC. NEC is a serious illness in very sick, usually premature newborns [Theo was not premature] but it happens when tissue in the large intestine (colon) becomes inflamed. No one knows what causes NEC. I remember finding out this information and looking at our core nurse practitioner at the time and saying: “This is bad… like this is really bad” She looked at me calmly and said “Jessica this is very bad but we’re treating it aggressively”. At this point in Theo’s journey, I was on auto-pilot and just kept pumping. During this whole time, no one said to me “Jessica it’s OK if you want to stop pumping”. No one once asked me how I was coping with all this while still managing to pump around the clock. The problem with having a critically ill baby is that everyone is taking care of the baby (which they obviously should be) but everyone forgets about the mama and her well-being and that is a huge problem. So I carried on and I continued pumping as I thought a diligent mother should. I started talking to other moms in the NICU and at Ronald McDonald House; we were all struggling with not sleeping due to stress, then when we could sleep, it was interrupted by our pumping schedule. So I started to test out longer stretches at night (which is forbidden in the pumping world) but it helped me get the restful sleep that I really needed. You do need to be very careful when you take longer stretches without pumping for the risk of infection. I found if I was able to get 7-8 pumps in during the day, I could go for a 6-7 hour stretch at night and then do a long pump in the morning. (And yes... you would probably never get a 7 hour sleep with a newborn but the fatigue of living in a hospital is unimaginably draining). 5. IF THE BABY ISN’T HAVING BREAST MILK OR FORMULA, WHAT IS IT “EATING?”: Babies who cannot orally feed are provided with TPN (Total Parenteral Nutrition) which is a mixture of vitamins that are altered each day to meet the changing needs of the baby. As well, the baby is fed Lipids which are a combination of fats for their body and brain to grow. Both TNP and Lipids were fed to the baby via their PICC line (refer to the what to expect section). SIDENOTE: At the two & a half month mark, Theo was still not consuming breast milk orally. Luckily, I had started producing healthy volumes of milk and I had a ton of breastmilk stocked up! So much so, that we were told by the freezer department of the hospital that we had to come and collect my milk because they had no more room for it. We actually had to buy a deep freezer for all the milk I had pumped! I am NOT mentioning that to gloat, but I am not pointing this out because I had A LOT of milk frozen and Theo was still NOT eating. I wondered again WHY was there so much pressure to keep pumping??? Why didn’t any health professional consult with me about my pumping? Why didn’t any health professional allude to the fact that Theo may eventually need formula to supplement with as he was gaining weight at an extremely slow rate. Regardless, I kept pumping. I truly believed that if I stopped I was a horrible and selfish mother. I was exhausted, mentally, physically and emotionally and now officially felt like a cow. 6. WHEN AND HOW TO START BREAST-FEEDING (if you can): Once your little babe starts successfully feeding from a bottle (and keeping it down), you may be encouraged to try breastfeeding. With Theo, my experience was extremely negative. Two years later with Christian, I found the hospital as a whole was collectively trying to promote breastfeeding (even if it was the smallest amounts) as soon as the baby was able to intake milk despite the range of health issues facing the baby. When I was on the surgical floor with Theo, the surgery team came by one morning on rounds and asked if I had tried breast-feeding. I said no I haven’t… “Like I’m just supposed to put him to my boob and he’ll eat?” The doctors casually looked at me and said “yeah”, just put him on your breast and see what happens”. Well needless to say that was a terrible idea, not to mention really traumatic. I was still learning and struggling to bond with Theo and this situation only added to my stress; I had no clue what I was doing and neither did Theo! At the time I felt like a complete failure. I had worked SO hard to establish a good milk supply to breast-feed and here I was trying to feed my baby and FAILING. This initial experience was so disappointing because I was not set up for success and if managed differently, it could have been far less traumatic. With Christian, I was encouraged to try breast-feeding as soon as he could start feeding orally. Even though Christian had a Nasel Cannula (basically tubes in his nose help to increase airflow), the lactation consultant encouraged and helped me place him on my breast even just for a couple minutes at a time. Then, as he was physically able to take in more milk and I became more comfortable, we slowly increased length. When trying breastfeeding for the first time, have a nurse or lactation consultant with you. They may not be available for your feeding/pumping schedule, but having support usually helps. If you need to wait, WAIT a feed and try at the next one with assistance. You may not always like who you get to work with; that's okay; ask for someone else! 7. PROCESS TO FEEDING AT HOME: THEO: When Theo started to intake larger volumes of milk, his reflux became out of control and he would vomit more than he would consume. Every time he would make small gains in consuming the correct amount of breastmilk, the volumes he would need to consume would increase as he was slowly getting bigger. This was exhausting and super stressful! I was alone in a small room and my only job was to feed my kid and he wouldn’t freaking eat. Feeding my kids will probably haunt me until the day I die. Theo definitely could feel the stress from me when feeding him and as a result, he ate better for my husband, family members or nurses who fed him and of course this REALLY PISSED ME OFF! It was my breast milk! I was his mother! Everyone else was feeding him better than I could and this only made me more depressed and anxious and less connected to Theo. At 4 months we were discharged with my copious amounts of frozen breast milk that we had to end up fortifying with formula to add needed calories to Theo’s diet. And guess what...I was advised to keep pumping at home! Don’t you think one brilliant mind could have mentioned: “Hey, Jessica, you have a shit ton of breast milk - why don’t you stop pumping so it’s one less thing for you to worry about when you get home”? Theo eventually needed an NG Tube and later a G-Tube to support his feeding. This experience is included in the TUBE feeding section. CHRISTAIN: Christian was able to breast-feed and progressed very well. As, mentioned prior, the whole team encouraged and positively supported me through the process. I would try to spend the WHOLE day at the bedside to improve breast-feeding independently. At the beginning, the nurses and I would weigh Christian before and after his feeds to see how much he ate (it literally was as suspenseful as The Biggest Loser TV Show weigh ins!). Christian was taking in the adequate volumes of milk throughout the day and night. Later, I would sleep overnight in the pumping rooms (which are outrageously unforgettable) and the nurses would call me at night to practice “on-demand” feeding (feeding when the baby wants to feed), opposed to feeding by the hour. I believe Christian was discharged directly from the NICU because, unlike Theo, there was less focus on a specific amount of milk consumed at each feed. It is also important to note that Christian’s gastroschisis was far less complex than his big brother’s and did typically feed well. With bottle feeding, it’s easier to see the amount of milk consumed than when exclusively breast-feeding as you are assuming the baby has eaten enough based on their mood and sleep. Unfortunately, despite all my best efforts, I stopped breastfeeding and pumping a month after being home. In the TUBE FEEDING section, I explain how I was in constant communication with medical staff regarding Theo’s milk consumption and despite the nurses reassuring me that Christian was feeding like a “typical” baby, I mentally couldn’t handle not knowing how much or little he was taking in. At the end of day, I truly believe a physically, emotionally and mentally HEALTHY mom is BEST for your baby and if that doesn’t include pumping or breastfeeding...THAT’S OKAY. Whether your baby is bottle fed with breast milk, bottle fed with fortified breast milk, bottle fed with no name formula, bottle fed with organic top of the line blah, blah, blah formula or breastfed...guess what - they are fed! What matters is that your baby is eating and growing...end then! |
To navigate the BTB blog, you can scroll through the posts, or if you're looking for something specific - you can click on a category below & it will take you to related posts!
••• k Archives
September 2022
Categories
All
|
 RSS Feed
RSS Feed