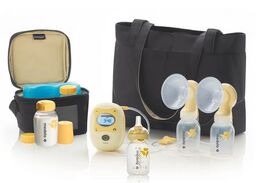
 Chapter One: Pumping My son Theo was born with gastroschisis, a birth defect in which the intestines grow outside the baby’s body. As soon as my son was born, even before I was able to see him, the nurses started talking to me about pumping. I was literally told “Jessica, your only job is to pump right now”. Theo’s condition was very complex and I felt completely helpless as his mother. I felt that the only thing I could really do for my baby was to pump and I soon found that pumping consumed my life and became a source of my anxiety. In saying that, I don’t regret pumping by any means BUT….at the same time I look back and wonder why was that enormous pressure placed on me? Every mom has to make the decision that’s right for her and her baby and while I choose to pump, you need to do what’s right for you. My experience with feeding Theo was traumatic and while I’m not trying to scare other mom’s who may be experiencing similar struggles, I want to provide recommendations and suggestions for pumping/breastfeeding that I wish I someone shared with me. I’m not a medical professional so all recommendations are just based on my personal experience. STEP 1: GET A PUMP AND A PUMPING BRA!!! Prior to pregnancy, buy a high quality pump. Many insurance plans cover them with a doctor's note when you have a high risk pregnancy. If purchasing one is not an option, they can be rented for a reasonable price from the hospital where they are sterilized daily. Learn how to use the pump BEFORE the baby comes out. DADDY/your partner: LEARN how to clean and sterilize the kit (as that will be a huge help for mama). I definitely didn’t do that the first time; I was trying to pump while learning how to put the damn thing together and I had no clue what the hell I was doing. After an untraditional birth the last thing you want to be dealing with is how to use the pump correctly. Prior to your induction/due date, explore the pump! Attach the pump with the correct cords and play with the settings. Then put it on your boobs - TEST IT OUT! Learn how to attach the pumping bra to the pump. I didn’t use a pumping bra until I got home from the hospital with Theo and it was a total game changer as you are hands free! The first setting will probably be uncomfortable for a while. However, once your milk starts coming in, you will be able to increase the suction comfortably. STEP 2: Buy a sterilization kit. I bought one that went in the microwave and really liked it because it was compact and easy to use. There are also disposable bags you can use that are convenient when on the go. Have all of this ready to go in advance. 3. WHEN TO START: Once you are settled after the birth and feel somewhat composed, try to put the pump on your breasts. With Theo I produced NOTHING for about three days. I was panicking and felt like a failure. At the same time, NO one was encouraging my efforts and reminding me that my situation was nowhere close to a normal experience. OF COURSE my milk wasn’t coming in; my baby was in critical care, literally fighting for his life and I was stressed beyond belief. It is important to remember women’s milk supply usually comes in because moms typically hold the baby after birth. With the stress of having your baby covered in tubes and wires, followed by a perhaps undesirable birth, it is only natural that your body responds by saying, WHAT THE FFF?! WHERE’S THE BABY??? I’M CONFUSED! You’ll most likely be told to put the pump on your breast every two hours. As a natural rule follower, I became obsessed with my exclusive pumping role and being on-time to the very minute to pump. Well guess what….after giving birth you might not be able to walk, you might not even be staying in your house and pumping rooms are not always available at the hospital when you want to pump. So all you can do is try your best to pump on the two hour mark. If you're 20 minutes or an hour behind, take a breath, you’re living through unimaginable time with your baby and it’s fine to move at your own pace. The nurses and lactation consultants will be asking you about pumping. Some are kinder than others. Remember this is YOUR experience, NOT theirs. Listen to your body and just keep trying your best. SIDENOTE: I’m not sure why our society doesn’t talk about this but breast-feeding/pumping is hard! It’s so hard that there are specialized trained nurses whose main role is to teach women how to breast-feed. Don’t get me wrong, there are multiple important and amazing parts of breast-feeding but I think we should highlight that if it was so damn easy and natural, why is it someone’s career to just teach women how to do it? 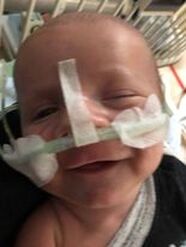 4. WHERE TO PUMP IN THE HOSPITAL: The NICU at Sick Kids is unimaginably small...hence the NEED for a new SickKids building. It’s recommended to pump by the bedside to improve milk production as you are in close proximity to your baby. Nurses can provide covers for privacy, don’t be afraid to ask. At first I was completely uncomfortable pumping by the bedside with Theo. I felt that the curtains didn’t give me enough privacy and I didn’t know what the hell I was doing. When my second born, Christian, was also born with gastroschisis and I found myself in the same situation, I often asked to pump by the bedside. I preferred it much more the second time around as I didn’t need to wait for a room, I could consistently pump on the approximate two hour mark during the day and I felt a little more connected to Christian when pumping. Also, the great thing about pumping beside the bedside is that you can provide mouth care to your baby immediately. Mouth care is provided when your baby is not receiving feedings by breast or bottle. You swab the inside of your baby’s mouth with small amounts of your colostrum then later breast milk. I really enjoyed doing this hands-on care for my boys and it helped me to feel connected to the boys and feeling like a mom. So many aspects of becoming a mom were taken away from me and this small experience helped me to feel like I was a mother and I could do something for my baby. Also my husband could participate in mouth care which provided a bonding experience for him as well. Both my boys did not receive milk from a bottle or breast until they were approximately two and a half months old. With regards to Theo, he went through a lot at the beginning; in the first four hours of his life, he needed an immediate surgery and my husband was told he may not make it. Doctors kept telling my husband and I that our son’s case was extremely complicated but after the first week, he started improving despite his unhealthy bowels outside his body. After the two week mark, we got a call in the middle of the night to come to the hospital right away. Theo needed a large blood transfusion and we were told he may not make it through the night. Later we were told he was septic, had E.Coli in his blood as well as a condition called NEC. NEC is a serious illness in very sick, usually premature newborns [Theo was not premature] but it happens when tissue in the large intestine (colon) becomes inflamed. No one knows what causes NEC. I remember finding out this information and looking at our core nurse practitioner at the time and saying: “This is bad… like this is really bad” She looked at me calmly and said “Jessica this is very bad but we’re treating it aggressively”. At this point in Theo’s journey, I was on auto-pilot and just kept pumping. During this whole time, no one said to me “Jessica it’s OK if you want to stop pumping”. No one once asked me how I was coping with all this while still managing to pump around the clock. The problem with having a critically ill baby is that everyone is taking care of the baby (which they obviously should be) but everyone forgets about the mama and her well-being and that is a huge problem. So I carried on and I continued pumping as I thought a diligent mother should. I started talking to other moms in the NICU and at Ronald McDonald House; we were all struggling with not sleeping due to stress, then when we could sleep, it was interrupted by our pumping schedule. So I started to test out longer stretches at night (which is forbidden in the pumping world) but it helped me get the restful sleep that I really needed. You do need to be very careful when you take longer stretches without pumping for the risk of infection. I found if I was able to get 7-8 pumps in during the day, I could go for a 6-7 hour stretch at night and then do a long pump in the morning. (And yes... you would probably never get a 7 hour sleep with a newborn but the fatigue of living in a hospital is unimaginably draining). 5. IF THE BABY ISN’T HAVING BREAST MILK OR FORMULA, WHAT IS IT “EATING?”: Babies who cannot orally feed are provided with TPN (Total Parenteral Nutrition) which is a mixture of vitamins that are altered each day to meet the changing needs of the baby. As well, the baby is fed Lipids which are a combination of fats for their body and brain to grow. Both TNP and Lipids were fed to the baby via their PICC line (refer to the what to expect section). SIDENOTE: At the two & a half month mark, Theo was still not consuming breast milk orally. Luckily, I had started producing healthy volumes of milk and I had a ton of breastmilk stocked up! So much so, that we were told by the freezer department of the hospital that we had to come and collect my milk because they had no more room for it. We actually had to buy a deep freezer for all the milk I had pumped! I am NOT mentioning that to gloat, but I am not pointing this out because I had A LOT of milk frozen and Theo was still NOT eating. I wondered again WHY was there so much pressure to keep pumping??? Why didn’t any health professional consult with me about my pumping? Why didn’t any health professional allude to the fact that Theo may eventually need formula to supplement with as he was gaining weight at an extremely slow rate. Regardless, I kept pumping. I truly believed that if I stopped I was a horrible and selfish mother. I was exhausted, mentally, physically and emotionally and now officially felt like a cow. 6. WHEN AND HOW TO START BREAST-FEEDING (if you can): Once your little babe starts successfully feeding from a bottle (and keeping it down), you may be encouraged to try breastfeeding. With Theo, my experience was extremely negative. Two years later with Christian, I found the hospital as a whole was collectively trying to promote breastfeeding (even if it was the smallest amounts) as soon as the baby was able to intake milk despite the range of health issues facing the baby. When I was on the surgical floor with Theo, the surgery team came by one morning on rounds and asked if I had tried breast-feeding. I said no I haven’t… “Like I’m just supposed to put him to my boob and he’ll eat?” The doctors casually looked at me and said “yeah”, just put him on your breast and see what happens”. Well needless to say that was a terrible idea, not to mention really traumatic. I was still learning and struggling to bond with Theo and this situation only added to my stress; I had no clue what I was doing and neither did Theo! At the time I felt like a complete failure. I had worked SO hard to establish a good milk supply to breast-feed and here I was trying to feed my baby and FAILING. This initial experience was so disappointing because I was not set up for success and if managed differently, it could have been far less traumatic. With Christian, I was encouraged to try breast-feeding as soon as he could start feeding orally. Even though Christian had a Nasel Cannula (basically tubes in his nose help to increase airflow), the lactation consultant encouraged and helped me place him on my breast even just for a couple minutes at a time. Then, as he was physically able to take in more milk and I became more comfortable, we slowly increased length. When trying breastfeeding for the first time, have a nurse or lactation consultant with you. They may not be available for your feeding/pumping schedule, but having support usually helps. If you need to wait, WAIT a feed and try at the next one with assistance. You may not always like who you get to work with; that's okay; ask for someone else! 7. PROCESS TO FEEDING AT HOME: THEO: When Theo started to intake larger volumes of milk, his reflux became out of control and he would vomit more than he would consume. Every time he would make small gains in consuming the correct amount of breastmilk, the volumes he would need to consume would increase as he was slowly getting bigger. This was exhausting and super stressful! I was alone in a small room and my only job was to feed my kid and he wouldn’t freaking eat. Feeding my kids will probably haunt me until the day I die. Theo definitely could feel the stress from me when feeding him and as a result, he ate better for my husband, family members or nurses who fed him and of course this REALLY PISSED ME OFF! It was my breast milk! I was his mother! Everyone else was feeding him better than I could and this only made me more depressed and anxious and less connected to Theo. At 4 months we were discharged with my copious amounts of frozen breast milk that we had to end up fortifying with formula to add needed calories to Theo’s diet. And guess what...I was advised to keep pumping at home! Don’t you think one brilliant mind could have mentioned: “Hey, Jessica, you have a shit ton of breast milk - why don’t you stop pumping so it’s one less thing for you to worry about when you get home”? Theo eventually needed an NG Tube and later a G-Tube to support his feeding. This experience is included in the TUBE feeding section. CHRISTAIN: Christian was able to breast-feed and progressed very well. As, mentioned prior, the whole team encouraged and positively supported me through the process. I would try to spend the WHOLE day at the bedside to improve breast-feeding independently. At the beginning, the nurses and I would weigh Christian before and after his feeds to see how much he ate (it literally was as suspenseful as The Biggest Loser TV Show weigh ins!). Christian was taking in the adequate volumes of milk throughout the day and night. Later, I would sleep overnight in the pumping rooms (which are outrageously unforgettable) and the nurses would call me at night to practice “on-demand” feeding (feeding when the baby wants to feed), opposed to feeding by the hour. I believe Christian was discharged directly from the NICU because, unlike Theo, there was less focus on a specific amount of milk consumed at each feed. It is also important to note that Christian’s gastroschisis was far less complex than his big brother’s and did typically feed well. With bottle feeding, it’s easier to see the amount of milk consumed than when exclusively breast-feeding as you are assuming the baby has eaten enough based on their mood and sleep. Unfortunately, despite all my best efforts, I stopped breastfeeding and pumping a month after being home. In the TUBE FEEDING section, I explain how I was in constant communication with medical staff regarding Theo’s milk consumption and despite the nurses reassuring me that Christian was feeding like a “typical” baby, I mentally couldn’t handle not knowing how much or little he was taking in. At the end of day, I truly believe a physically, emotionally and mentally HEALTHY mom is BEST for your baby and if that doesn’t include pumping or breastfeeding...THAT’S OKAY. Whether your baby is bottle fed with breast milk, bottle fed with fortified breast milk, bottle fed with no name formula, bottle fed with organic top of the line blah, blah, blah formula or breastfed...guess what - they are fed! What matters is that your baby is eating and growing...end then!
0 Comments
 With both pregnancies, I received prenatal care at the High-Risk Clinic at Mount Sinai Hospital in Toronto. Once my sons were born, they were immediately attended to by a Sick Kids team working remotely out of Mount Sinai. The team worked until they were stable and then they were directly transferred to the Hospital for Sick Children. Mount Sinai Hospital and the Hospital for Sick Children are world renowned hospitals. The reputations, as well as the team’s working with my family, made me feel 100% at ease. The hospitals work collaboratively to provide frequent meetings for families. The meetings included both the Mount Sinai OBs and a Sick Kids team to explain the plan, what to expect, and answer any questions or fears I had. At the time I was terrified but felt as prepared as I could be. Now that I’ve gone through the experience, I believe that knowledge is power. The more you know going into a difficult situation, the better coping may be. Since I’ve beaten the perceived impossible odd and had two babies with Gastrochisis, I believe that my story can help fully prepare families with what to expect. As mentioned in my intro, the hardest part for me was - and sometimes still is - the feeling of loneliness. This guide is solely based on my experiences and any medical explanations are from my perspective. The purpose of sharing these points is to help parents become ready and aware for the, sometimes very difficult, journey ahead of them. Below I’ve lists factors that I believe are important know. That said, I want to point out that both my children’s conditions were complex and were not a typical Gastrochisis cases. In fact, it was explained to my husband and I that Theo, our first born, was one of the worst cases of Gastrochisis Sick Kids has ever seen. His first surgery was at 4 hours old and my husband was told he may not survive the surgery. I am noting this grim point because my boys went through the worst of it, and now they’re healthy and thriving. Remember, you will get through this: 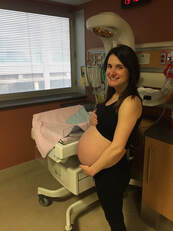 What to expect and what helped me get though it:
What helped me get through it: Having my spouse or a family member come with me. Despite having such thorough care, being pregnant with a sick baby is terrifying! I know how hard it is for a spouse to take so much time off from work, but you don’t have to go through this alone. Reach out to others. And if no one can come with you physically, tell a loved one when your appointments are and have them check in on you. Consider a FaceTime after the ultrasound or have someone come over for dinner the evening of. Also - SNACKS! Oh man, when you think you have packed enough, add at least 2 more foods to your food bag and 1 more drink! Some appointments were terribly long. Bring something to keep you mind off your appointment other than your phone. Examples include, a book, magazines, downloaded shows, etc. The internet connection wasn’t the greatest, so tangible distractions were helpful. 2. Expect: You may be a complete basket case when the baby is born What most people don’t realize in a Gastrochisis pregnancy is that women are able to have a vaginal birth. Keep in mind, this does depend on your hospital. Since I was being cared for by Mount Sinai and The Hospital for Sick Children, they had specialized staff who can readily handle complex births. If you live in an area where a team needs to be coordinated, you may have a planned c-section. Also, when having a baby with Gastrochisis, you are induced at 37 weeks. Being induced isn’t fun to say the least, but it wasn’t as bad as I thought. There are two ways a woman can be induced. One with a gel and the second is with a foley catheter. For me, the gel was much more pleasant. My experience with the foley catheter was very painful, so if you have the option go for the gel! As well, it was explained to me that if an average healthy pregnancy were to be induced at 37 weeks, most babies would go into distress and need an emergency C-section. But for Gastrochisis babies, they are able to be born vaginally due to an increase in amniotic fluid.  Literally right answer I gave birth to Christian Literally right answer I gave birth to Christian For both my births, I had the OB team and Sick Kids team in the surgical room. This means A LOT of doctors, so be prepared to leave your pride at the door because a whole lot of people are going to be looking at your vagina. Once the baby comes out, you may have a quick peek at your new pride and joy and then the baby will be taken to the adjacent room where the pediatric team will get them stable. Once stable, I was able to have a quick visit with them and then they were taken to Sick Kids. Once YOU are somewhat stable, a transport team take you over in a wheelchair to see your baby. Having a baby under normal circumstances is emotional, but when you’re seeing your baby for the first time and they’re in critical state it can be overwhelming to say the least. Then to see your babe stable but covered with wires and tubes is a whirlwind of emotions. I was happy, I was scared, I was exhausted, I was physically in a lot of pain, and I had so many questions but could not get the words out. I wasn’t able to hold either of my boys for weeks. Something that I am slowly starting to share with others is that I didn’t feel a connection to either of my boys when they were first born. I’ve discovered that this was a coping mechanism. I believe that if my baby died, at least I wasn’t bonded with him. YES, this is some dark and scary shit! But it’s important to be honest and open up about my experience in the hopes of helping others. What helped me get through it: Have people come see you! With Theo (my eldest) I didn’t want anyone at the hospital as I thought it was weird to have visitors with an NICU baby. For me this was not a joyous and exciting time, I was terrified and felt so ripped off of my experience. However, the second time around, when I had Christian, I planned for my sister to be with me as soon as he came out so my husband could immediately go to Sick Kids with the baby. The first time, my dad - God bless him - was the only around during my episiotomy…blah! I’m extremely close with my sister and she is able to make anything into a joke. Her support and help after the birth was comforting and put me in a positive headspace. I recommend having a family member or friend there to support BOTH parents. No matter how much you prepare yourself for this moment, you never know how you will react until you’re in it. And remember, no reaction is right or wrong. Be kind to yourself and don’t forget that this too shall pass… 3. Expect: Not to pack a transitional hospital bag. There is so much information out there on how to pack the “perfect” hospital bag. But this looks very different when having a sick baby. What helped me get through it: STOP following mommy blogs, magazines for mommies to be, etc. Most healthy pregnancy experiences are much different than what I experienced. By removing the comparison of what I thought having a baby would be like was extremely helpful for me. Things you need to pack: For both babies, I stayed at the Ronald McDonald House in Toronto. Sometimes you get in immediately and other times you need to wait - depending on the availability of the house. Both times, my husband and I packed a month’s supply of comfy clothing and personal care items that we left in the car.
Items for my baby: The first time around, I was very upset as the hospital bag I had packed for my baby wasn’t helpful or useful. I couldn’t use anything I packed in the bag and I believe this further increased my disconnection with the baby. As well, not to discredit any of my amazing family or friends, but many generous gifts we were given to us in the hospital so they couldn’t be used. Instead of gifts bringing new parents joy, many gifts added to an already very stressful situation as we couldn’t use most items. The second time around, I thought very hard about what items I could use right away.
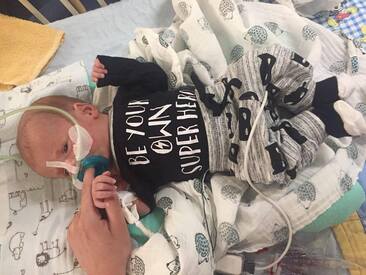 Christian's first outfit put on my mama <3 Christian's first outfit put on my mama <3 4. Baby’s first outfit Unfortunately, I had a pretty negative experience with my eldest son, Theo, regarding his first outfit. To date, I have great relationships with many of the incredible nurses who cared for my boys. We often communicate over social media and I love staying connected with them. When you are in the hospital for such a long time, your nurses not only become your friends but feel like family. Like all situations in life, you’re not going to become friends and like everyone you meet and work with, so of course this was true with our nurses. Once Theo’s intestines were in his stomach, it didn’t occur to me to bring clothes to the hospital to dress him in. For two months prior, he was just in a diaper and wearing socks and a hat. Like many new moms, I had a special outfit picked out for him that I had hoped to dress him in it. I came to the hospital one morning and a nurse (one who I did not have a good relationship with) had dressed him in used hospital clothing. Her intentions were in the right place and honestly if another nurse dressed him, I probably wouldn’t have been so upset. However, when you’re already had issues conceiving, followed by a complex pregnancy and then a critically ill child, you feel you have been robbed of so much. This was something I was greatly looking forward to and I was devastated to see my baby dressed, not only by someone I did not like but on top of that, in used hospital clothes. Something you CAN do: The second time around I explained my past experience to a nurse I had a close relationship with. She validated my experience and suggested that I hang Christian’s outfit on the side of the crib. At the beginning, I didn’t want to do it as I was still really upset about my last experience. But hanging the outfit and seeing it there daily ended up being a positive thing for me. It gave me hope that Christian would soon be healthy, and I would be able to hold him in the near future. It also helped me feel like a mom and that I was somewhat in control of my situation. I highly recommend still bringing your baby’s first outfit along with the hanger and having it near the isolate (an isolate is like an incubator as it keeps the baby warm, but they’re not completely covered). 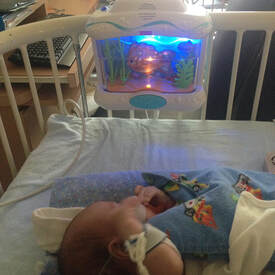 Items to have nearby:
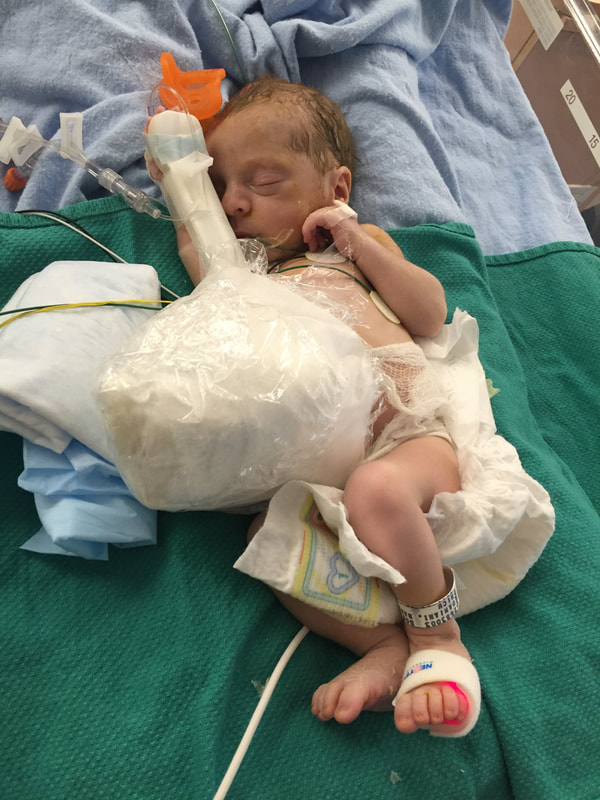
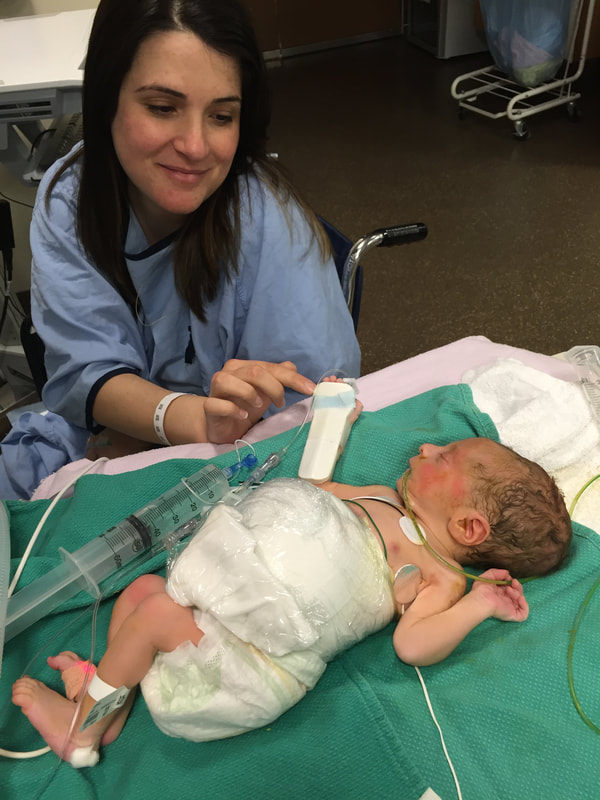
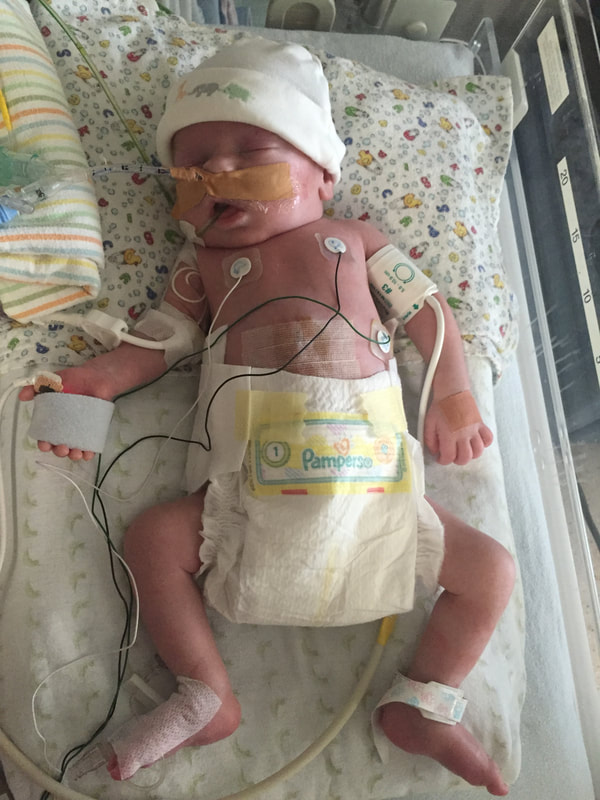
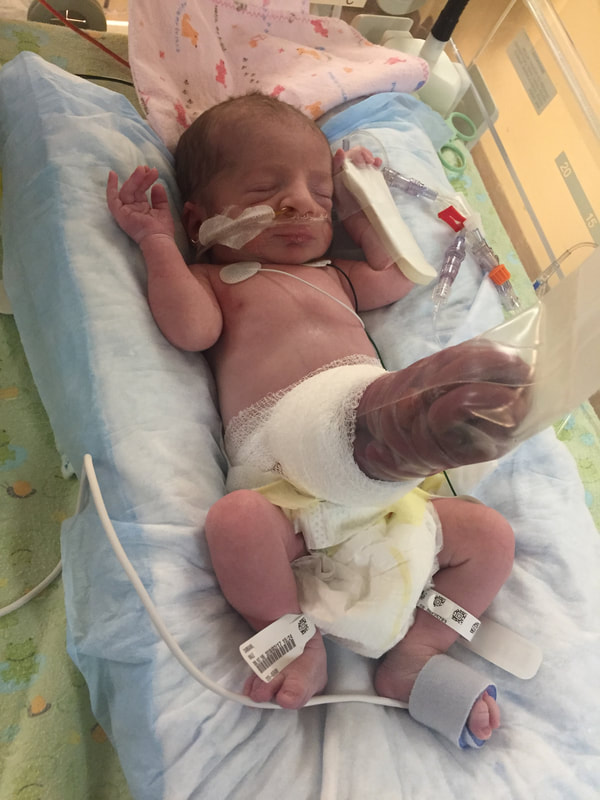
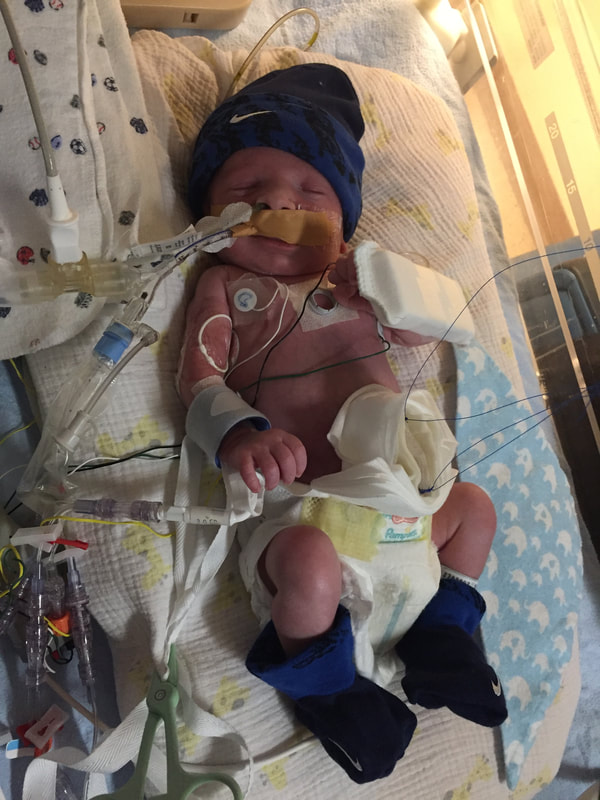
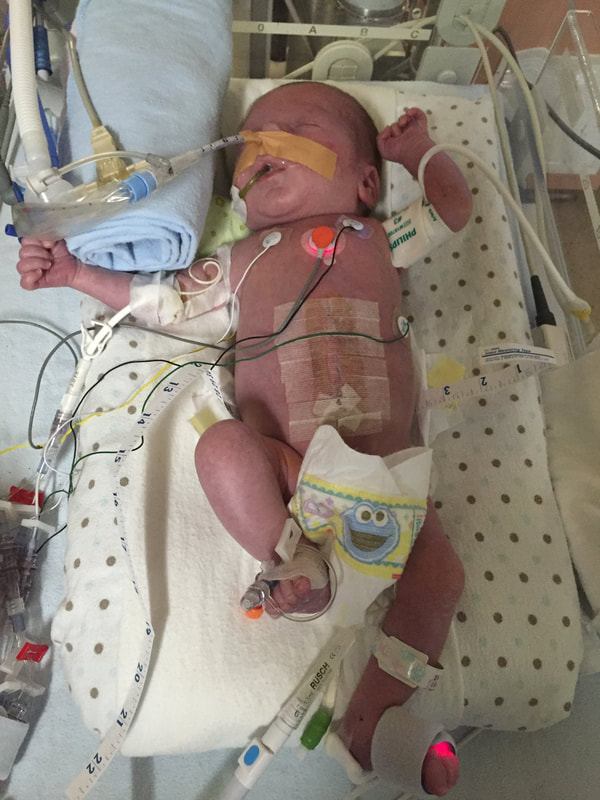
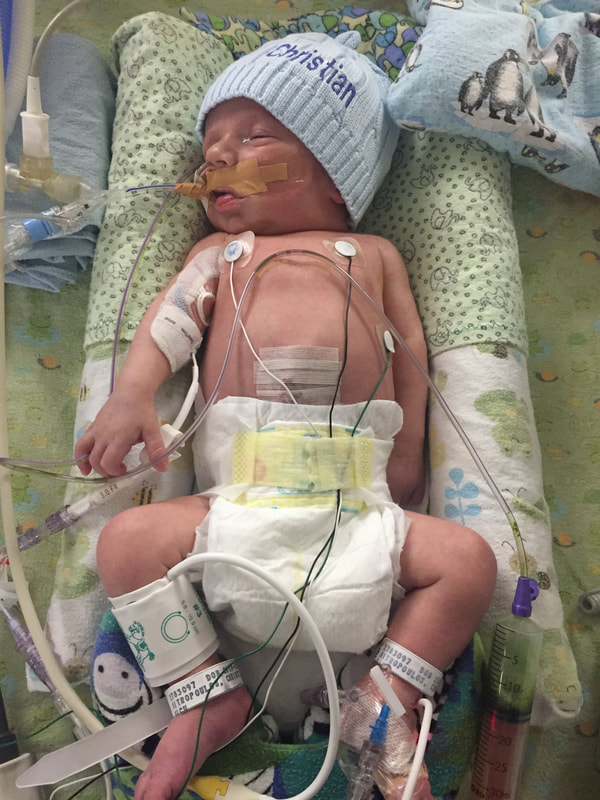
5. Medical procedures that will probably happen: As I mentioned in this section, Mount Sinai and Sick Kids work together and set up meetings with in hopes of preparing parents prior to having their sick baby. From going through my experience TWICE, the NICU is all I know. During this difficult time, transparence is key. I believe if I was prepared more with the ugly truth of what to really expect, perhaps the first time around, our experience may have been less traumatic. In my opinion, the best way to fight fear is with information. When reading through this list remember that most medical procedures that happen on your baby are completely terrifying. But if you are expecting them to take place, then they may be less overwhelming. I was prepared for the ugly reality of the NICU the second time around and procedures were far less daunting, as I expected them and knew they were part of the process. How the heck does their intestines go back in? Once your beautiful babe comes out, a pediatric team will immediately start to care for your baby in a separate room. In my case, the room was attached to the delivery room. You will see your baby once they’re stable from the birth and the intestines are cleaned. When I saw my eldest, I remember thinking he looked like a mummy from ancient Egypt - his stomach was completely rapped up with white gauze. Your baby with also have an IV started and an NG tube, which will be explained later. Obviously, this is probably not the idea you had in mind when you found out you were expecting. To be honest, this part wasn’t as scary as I thought it would be. Everything was so surreal; I don’t know how, but I just went with the motions. [Note: to this day, I still struggle when seeing pictures of new mom’s holding their babies. I don’t think I will ever enjoy a Pampers commercial and I can feel my stomach turn when I hear positive labour stories. I am no longer angry about my story, but I think I will always be sad that I could not hold by baby for so long…and I’m learning that these feelings that have stuck with me are valid]Once your baby is safe to transfer, they will be taken to Sick Kids. Now their intestines will look different. Typically, the intestines are in a clear bag attached to a string, which is then attached to a C shaped bar that anchors overs your baby’s isolate. This allows for gravity to start making room for the intestines to descend into the stomach. Our eldest son’s case was very complicated, and his intestines were in bad shape when he was born. During his treatment, a surgical nurse showed me a picture of what his intestines looked like immediately after birth and it was grotesque! The intestines enter the body in 3 steps: 1) Gravity: as the baby is laying of its back, gravity encourages the intestines to naturally descend into the stomach. 2) Reductions: the surgical team would come by every couple of days and depending on how the baby is doing, they would slowly squeeze the bag or push down on the intestines. This is quick but can be painful and for this reason babies are given pain medication. 3) Surgery: Once the intestines are very close to the stomach wall, they will bring surgically stitched back together. Pictures: In recent years, I only started sharing pictures of my babies’ condition. I used to be terrified of other people these pictures. I imagined them sharing them to their friends and family as if they were a learning exhibit. But now, I believe it is extremely important to show images of what this condition really could look like. Parents need to understand and prepare themselves for what to expect. For me, I saw a picture of a baby with their intestines in a bag at the high-risk clinic at Mount Sinai Hospital. Even though it was only one picture, and it was quite dated, I found it very helpful. Not only seeing the typical size of the baby (both boys were approximately 5.5 lbs) it was helpful for me to visualize what it looks like to have a baby with intestines outside their body. Even NOW posting these pictures I have NEVER shared until now, bring tears to my eyes....  NG-Tube Once your baby is born, they will immediately have an NG tube placed on the inside of their mouth or nose. Because their intestines are outside the body, the NG tube helps to remove all the bile/waste out. To this day it breaks my heart when I see a Sick Kids advertisement showing a baby with my NG tube. As I will talk about later, Theo, had a lot of problems with feeding and had an NG tube for some time. Christian, our second child, only had it for the first two months at the hospital and did awesome at feeding once it was removed. Once the tube is placed inside your little babe, rest assured that they usually are quite comfortable. Seeing the tube go in that can be quite distressing. Remember most kiddos will only have the tube for a short period of time. PICC A couple days after Theo was born, we were told they would need a PICC. A what???? It was explained to me that this is a long-term IV that helps the baby directly get the nutrients. Your baby will not eat until their intestines are inside their body and once they are inside, they will very slowly start to drink breastmilk through either a NG tube, breast and or bottle. There are two ways a baby can have a PICC placed inside them. It can be done by a specialized nurse in the NICU or alternatively, the baby can be taken down to IGT where a paediatric radiologist uses diagnostic imaging to guide the PICC into place. For either procedures, your baby will be sedated. When we were first told that Theo would need a PICC we were completely terrified about the procedure and honestly, I thought he would die having it done. At the time, this procedure seemed extremely scary and daunting. However, once the PICC has been placed, it’s actually a great thing because it reduces the amount of times a baby is getting poked with an IV. With a PICC, doctors will have IV access and therefore need far less poking. The second time around, it was not stressful as we were prepared for this step and knew it was part of the process. We also asked and advocated for Christian to get a PICC immediately to reduce IV poking. Blood transfusion: Babies often need blood, especially before surgery to top up their hemoglobin as a precautionary measure. I’m not sure about you but, prior to this experience, when I heard “blood transfusion” I automatically thought someone was dying and they needed blood to live. I actually once said that to a nurse, and she laughed because it was such an inaccurate explanation of why babies need blood in the NICU. As mentioned prior, Theo‘s recovery in the hospital was very rocky. The first week he was doing well, as his intestine slowly were placed back into his stomach but then the second week, he developed NIC and E.coli in his blood. Not only were his intestines extremely dilated but these infections were life-threatening. One day we got a call at around 3am that Theo needed blood. It was one of the scariest nights as we didn’t know what state he would be in when we got to the hospital. Seeing a very pale sick baby being pumped with blood is terrifying, even if it is only a precautionary measure. A beautiful thing happened in our NICU room. As most people are aware, The Hospital for Sick Children is in the process of building a new hospital. The current NICU is extremely tight space. There is tape on the floor around your baby’s crib to indicate your space, so there is very little privacy between you and other families. That said, being in such close proximity to other people in the same situation as you can sometimes be a blessing. When Theo was hooked up with blood and quite critical, we started talking to the parents next to us. The mom said, “I know it’s scary to have blood hooked-up to your baby but honestly they do it all the time here.” She told me that her baby already had three transfusions. I remember looking at her like she was speaking another language but having her reassurance that this was part of the process was so comforting. Needless to say, it was an automatic friendship that we still have today. Intubation Intubation is when a breathing tube is placed down your baby’s throat and into their lungs to help them breathe. I’m going to be brutally honest with you; this is something very hard to prepare for. Babies, particularly babies with Gastro, need to be intubated because as their intestines are slowly pressed into their stomach so this puts a lot of pressure on the lungs and makes it difficult to breathe. Also, since the intestines are slowly being pushed into the stomach, your baby will be on a higher dose of pain medication which sometimes makes the lungs “lazy” and impacts breathing. Theo was intubated and extubated several times, but Christian was fully intubated for six weeks. The second time around, when Cristian was intubated, we were called and told it was going to happening. I anticipated this step in the process, but it was still hard to hear. Although Christian was in a much better situation then Theo, my husband started bawling when he heard the news. I can remember the call from in our nurse practitioner like it was yesterday. When your baby is intubated, they try to keep them as comfortable as possible but it’s still very hard to see. Despite this process being incredibly hard to deal with, I think it’s important to know that this is expected and needed in order for your baby to recover. I would like to make a side note about intubation; as mentioned prior, we had some touch and go moments with Theo. There was a situation where he needed to be intubated rather quickly. At this time, my husband and I were given the option to stay in the room. I understand why the option is given to parents, however, after going through the distressful situation I truly believe parents should not be allowed to stay in the room. I have advocated this to the NICU and understand it is a divided issue. I strongly advise any parent to remove yourself from the room during this procedure. The nurses, RT’s and doctors are experts. They know what they’re doing. They know that baby will look distressed during this process and they know the perfect steps of securing the breathing tube in place. During this procedure, my husband and I were both crying, and I ran out of the room and threw up. Breathing tube insertion are not fun. Once they’re in though, they are somewhat manageable to deal with. |
To navigate the BTB blog, you can scroll through the posts, or if you're looking for something specific - you can click on a category below & it will take you to related posts!
••• k Archives
September 2022
Categories
All
|


 RSS Feed
RSS Feed